Malaria, a life-threatening disease caused by “Plasmodium” parasites, remains one of the most significant global health challenges. Transmitted through the bites of infected female “Anopheles” mosquitoes, malaria affects millions of people annually, particularly in tropical and subtropical regions. Despite substantial progress in prevention and treatment, the disease continues to exert a heavy toll on public health, especially in low-income countries. This article provides a detailed overview of malaria, including its etiology, transmission, clinical manifestations, diagnosis, treatment, and prevention strategies.
Etiology and Transmission
Malaria is caused by protozoan parasites of the genus “Plasmodium“. Five species are known to infect humans: “Plasmodium falciparum”, ”Plasmodium vivax”, “Plasmodium ovale”, ”Plasmodium malariae“, and ”Plasmodium knowlesi“. Among these, ”P. falciparum“ is the most virulent and responsible for the majority of malaria-related deaths, while “P. vivax” is the most geographically widespread.
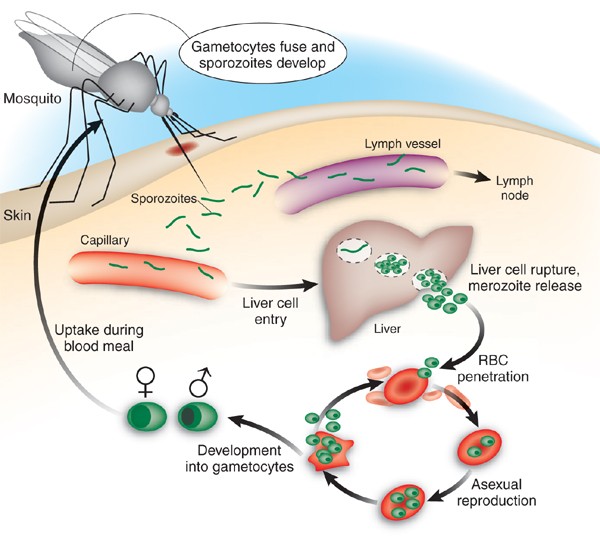
The life cycle of the malaria parasite involves two hosts: humans and “Anopheles” mosquitoes. When an infected mosquito bites a human, it injects sporozoites into the bloodstream. These sporozoites travel to the liver, where they mature and multiply into merozoites. The merozoites then invade red blood cells, initiating the erythrocytic cycle, which is responsible for the clinical symptoms of malaria. Some parasites differentiate into sexual forms (gametocytes), which can be taken up by another mosquito during a blood meal, completing the transmission cycle.
Clinical Manifestations
The symptoms of malaria typically appear 10–15 days after the infective mosquito bite. The classic presentation includes fever, chills, headache, and muscle pain, often accompanied by nausea, vomiting, and fatigue. These symptoms can be cyclical, corresponding to the rupture of infected red blood cells and the release of merozoites.
Severe malaria, predominantly caused by “P. falciparum”, can lead to complications such as cerebral malaria, severe anemia, acute respiratory distress syndrome, and multi-organ failure. “P. vivax” and “P. ovale” can form dormant liver stages (hypnozoites), which can reactivate weeks or months after the initial infection, causing relapses.
Diagnosis
Accurate and timely diagnosis is critical for effective malaria management. Microscopic examination of blood smears remains the gold standard for diagnosis, allowing for the identification of the parasite species and quantification of parasitemia. Rapid diagnostic tests (RDTs), which detect specific malaria antigens, are widely used in resource-limited settings due to their ease of use and quick results.
Molecular techniques, such as polymerase chain reaction (PCR), offer high sensitivity and specificity and are particularly useful for species differentiation and detecting low-level parasitemia. However, these methods require specialized equipment and expertise, limiting their use in endemic areas.
Treatment
The treatment of malaria depends on the species of “Plasmodium”, the severity of the disease, and the drug resistance patterns in the region. Artemisinin-based combination therapies (ACTs) are the first-line treatment for uncomplicated “P. falciparum” malaria. ACTs combine a fast-acting artemisinin derivative with a longer-acting partner drug to ensure complete parasite clearance and reduce the risk of resistance.
For severe malaria, intravenous or intramuscular artesunate is the treatment of choice, followed by a full course of ACT once the patient can tolerate oral medication. “P. vivax” and “P. ovale” infections require additional treatment with primaquine to eliminate hypnozoites and prevent relapses. However, primaquine can cause hemolysis in individuals with glucose-6-phosphate dehydrogenase (G6PD) deficiency, necessitating screening before administration.
Prevention and Control
Malaria prevention relies on a combination of vector control, chemoprophylaxis, and community engagement. Insecticide-treated bed nets (ITNs) and indoor residual spraying (IRS) are highly effective in reducing mosquito bites and transmission. Long-lasting insecticidal nets (LLINs) have been particularly successful in lowering malaria incidence in endemic regions.
Chemoprophylaxis is recommended for travelers to malaria-endemic areas. Drugs such as atovaquone-proguanil, doxycycline, and mefloquine are commonly used, depending on the destination and individual health considerations.
Vaccination represents a promising tool in the fight against malaria. The RTS,S/AS01 vaccine, which targets “P. falciparum”, has been shown to provide partial protection in children and is being piloted in several African countries. Ongoing research aims to develop more effective vaccines with broader coverage.
Challenges and Future Directions
Despite significant progress, malaria control faces several challenges. Drug resistance, particularly to artemisinin and its partner drugs, threatens the efficacy of current treatments. Insecticide resistance in “Anopheles” mosquitoes also undermines vector control efforts. Additionally, limited healthcare infrastructure and socioeconomic factors hinder access to prevention and treatment in many endemic regions.
Addressing these challenges requires a multifaceted approach, including sustained investment in research, innovation, and healthcare systems. Strengthening surveillance, promoting community-based interventions, and fostering international collaboration are essential to achieving the global goal of malaria elimination.
Conclusion
Malaria remains a formidable public health challenge, particularly in resource-limited settings. Understanding the biology, transmission, and clinical aspects of the disease is crucial for effective prevention and treatment. While significant strides have been made, continued efforts are needed to overcome the barriers to malaria control and ultimately eradicate this ancient scourge. Through a combination of scientific innovation, political commitment, and community engagement, the vision of a malaria-free world can become a reality.
We baysenmedical can supply Malaria rapid test kit with the above list.
Diagnostic Kit for malaria PF.PAN rapid test
Diagnostic Kit for malaria P.F/P.V rapid test
Diagnostic Kit for malaria PF rapid test
Welcome to contact for more details if you have demand!
Post time: Mar-12-2025